Serum Immunoglobulin G and M Levels in Attention Deficit Hyperactivity Disorder Children
Main Article Content
Abstract
Background and Objective: Inflammation and immune response are focused on recently for their possible role in development and pathophysiology of different neuropsychiatric disorders as Attention Deficit Hyperactivity Disorder (ADHD). However, a limited data is present within this research area. Different inflammatory markers could be associated with disease development. The objective of the study is to clarify the role of IgG & IgM in ADHD patients through measuring serum levels of these markers.
Methods: a case-control study that included 90 participants, 45 as patients’ group of ADHD with age range 6-12 (35 males and 10 females), in addition to 45 healthy control group. Serum levels of IgM and IgG were measured by using ELISA test.
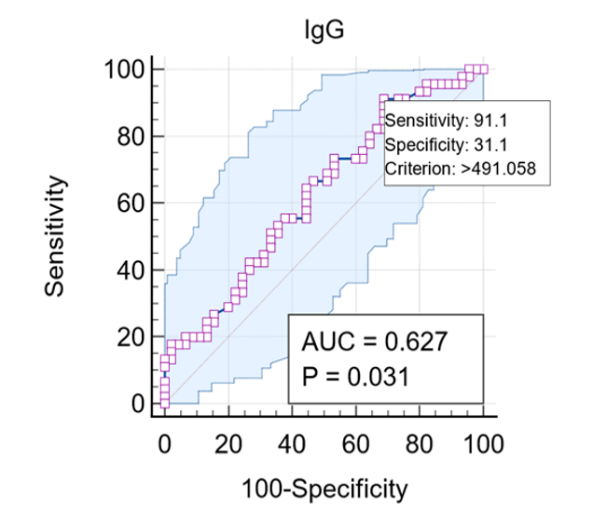
Results: a significant association between elevated serum level of IgG antibody and ADHD patients was reported. In addition, significant diagnostic utility for IgG. while no significant association with IgM levels were found.
Conclusion: the study concludes higher serum level of IgG which could be used as diagnostic biomarker for differentiating ADHD children from healthy children.
Article Details
References
Allan, S. M., & Rothwell, N. J. (2001). Cytokines and acute neurodegeneration. Nature Reviews Neuroscience, 2(10), 734–744. https://doi.org/10.1038/35094583
American psychiatric association diagnostic and statistical manual of mental disorders (5th ed., Vol. 41). (2003). American Psychiatric Publishing; Arlington, VA, USA.
Bekdas, M., Tufan, A. E., Hakyemez, I. N., Tas, T., Altunhan, H., Demircioglu, F., Kısmet, E., & Abant Izzet Baysal University Faculty of Medicine. (2014). Subclinical immune reactions to viral infections may correlate with child and adolescent diagnosis of attention-deficit/hyperactivity disorder: A preliminary study from Turkey. African Health Sciences, 14(2), 439–445. https://doi.org/10.4314/ahs.v14i2.21
Buske-Kirschbaum, A., Schmitt, J., Plessow, F., Romanos, M., Weidinger, S., & Roessner, V. (2013). Psychoendocrine and psychoneuroimmunological mechanisms in the comorbidity of atopic eczema and attention deficit/hyperactivity disorder. Psychoneuroendocrinology, 38(1), 12–23. https://doi.org/10.1016/j.psyneuen.2012.09.017
Donfrancesco, R., Nativio, P., Di Benedetto, A., Villa, M. P., Andriola, E., Melegari, M. G., Cipriano, E., & Di Trani, M. (2020). Anti-Yo Antibodies in Children With ADHD: First Results About Serum Cytokines. Journal of Attention Disorders, 24(11), 1497–1502. https://doi.org/10.1177/1087054716643387
Erşan, E. E., Doğan, O., Doğan, S., & Sümer, H. (2004). The distribution of symptoms of attention-deficit/hyperactivity disorder and oppositional defiant disorder in school age children in Turkey. European Child & Adolescent Psychiatry, 13(6), 354–361. https://doi.org/10.1007/s00787-004-0410-2
Giana, G., Romano, E., Porfirio, M. C., D’Ambrosio, R., Giovinazzo, S., Troianiello, M., Barlocci, E., Travaglini, D., Granstrem, O., Pascale, E., Tarani, L., Curatolo, P., Laviola, G., & Adriani, W. (2015). Detection of auto-antibodies to DAT in the serum: Interactions with DAT genotype and psycho-stimulant therapy for ADHD. Journal of Neuroimmunology, 278, 212–222. https://doi.org/10.1016/j.jneuroim.2014.11.008
Hassan, W., Noreen, H., Castro-Gomes, V., Mohammadzai, I., da Rocha, J. B. T., & Landeira-Fernandez, J. (2016). Association of Oxidative Stress with Psychiatric Disorders. Current Pharmaceutical Design, 22(20), 2960–2974. https://doi.org/10.2174/1381612822666160307145931
Howren, M. B., Lamkin, D. M., & Suls, J. (2009). Associations of depression with C-reactive protein, IL-1, and IL-6: A meta-analysis. Psychosomatic Medicine, 71(2), 171–186. https://doi.org/10.1097/PSY.0b013e3181907c1b
Instanes, J. T., Halmøy, A., Engeland, A., Haavik, J., Furu, K., & Klungsøyr, K. (2017). Attention-Deficit/Hyperactivity Disorder in Offspring of Mothers With Inflammatory and Immune System Diseases. Biological Psychiatry, 81(5), 452–459. https://doi.org/10.1016/j.biopsych.2015.11.024
Kemper, A. R., Maslow, G. R., Hill, S., Namdari, B., Allen LaPointe, N. M., Goode, A. P., Coeytaux, R. R., Befus, D., Kosinski, A. S., Bowen, S. E., McBroom, A. J., Lallinger, K. R., & Sanders, G. D. (2018). Attention Deficit Hyperactivity Disorder: Diagnosis and Treatment in Children and Adolescents. Agency for Healthcare Research and Quality (US). http://www.ncbi.nlm.nih.gov/books/NBK487761/
Krahel, A., Paszynska, E., Slopien, A., Gawriolek, M., Otulakowska-Skrzynska, J., Rzatowski, S., Hernik, A., Hanć, T., Bryl, E., Szczesniewska, P., Bilska, K., Duda, J., Tyszkiewicz-Nwafor, M., & Dmitrzak-Weglarz, M. (2021). Stress/Immune Biomarkers in Saliva among Children with ADHD Status. International Journal of Environmental Research and Public Health, 18(2), E769. https://doi.org/10.3390/ijerph18020769
Kronfol, Z. (2000). Cytokines and the Brain: Implications for Clinical Psychiatry. American Journal of Psychiatry, 157(5), 683–694. https://doi.org/10.1176/appi.ajp.157.5.683
Lam, A. P., de Sordi, D., Müller, H. H. O., Lam, M. C., Carl, A., Kohse, K. P., & Philipsen, A. (2020). Aggravation of symptom severity in adult attention-deficit/hyperactivity disorder by latent Toxoplasma gondii infection: A case-control study. Scientific Reports, 10(1), 14382. https://doi.org/10.1038/s41598-020-71084-w
Leffa, D. T., Torres, I. L. S., & Rohde, L. A. (2018). A Review on the Role of Inflammation in Attention-Deficit/Hyperactivity Disorder. Neuroimmunomodulation, 25(5–6), 328–333. https://doi.org/10.1159/000489635
Miller, B. J., Buckley, P., Seabolt, W., Mellor, A., & Kirkpatrick, B. (2011). Meta-analysis of cytokine alterations in schizophrenia: Clinical status and antipsychotic effects. Biological Psychiatry, 70(7), 663–671. https://doi.org/10.1016/j.biopsych.2011.04.013
Modabbernia, A., Taslimi, S., Brietzke, E., & Ashrafi, M. (2013). Cytokine alterations in bipolar disorder: A meta-analysis of 30 studies. Biological Psychiatry, 74(1), 15–25. https://doi.org/10.1016/j.biopsych.2013.01.007
Noori, M. A., AL-Hasnawi, S. M. J., AL-Haidari, A. F., & Hamza, D. M. (2020). Toxoplasma Gondii Seropositivity and Attention Deficit Hyperactivity Disorder. Journal of Global Scientific Research (ISSN: 2523-9376), 10, 871–879.
Passos, I. C., Vasconcelos-Moreno, M. P., Costa, L. G., Kunz, M., Brietzke, E., Quevedo, J., Salum, G., Magalhães, P. V., Kapczinski, F., & Kauer-Sant’Anna, M. (2015). Inflammatory markers in post-traumatic stress disorder: A systematic review, meta-analysis, and meta-regression. The Lancet. Psychiatry, 2(11), 1002–1012. https://doi.org/10.1016/S2215-0366(15)00309-0
Pollak, T. A., Drndarski, S., Stone, J. M., David, A. S., McGuire, P., & Abbott, N. J. (2018). The blood-brain barrier in psychosis. The Lancet. Psychiatry, 5(1), 79–92. https://doi.org/10.1016/S2215-0366(17)30293-6
Réus, G. Z., Fries, G. R., Stertz, L., Badawy, M., Passos, I. C., Barichello, T., Kapczinski, F., & Quevedo, J. (2015). The role of inflammation and microglial activation in the pathophysiology of psychiatric disorders. Neuroscience, 300, 141–154. https://doi.org/10.1016/j.neuroscience.2015.05.018
Riazi, K., Galic, M. A., Kuzmiski, J. B., Ho, W., Sharkey, K. A., & Pittman, Q. J. (2008). Microglial activation and TNFalpha production mediate altered CNS excitability following peripheral inflammation. Proceedings of the National Academy of Sciences of the United States of America, 105(44), 17151–17156. https://doi.org/10.1073/pnas.0806682105
Romanos, M., Gerlach, M., Warnke, A., & Schmitt, J. (2010). Association of attention-deficit/hyperactivity disorder and atopic eczema modified by sleep disturbance in a large population-based sample. Journal of Epidemiology and Community Health, 64(3), 269–273. https://doi.org/10.1136/jech.2009.093534
Schmitt, J., Apfelbacher, C., Chen, C.-M., Romanos, M., Sausenthaler, S., Koletzko, S., Bauer, C.-P., Hoffmann, U., Krämer, U., Berdel, D., von Berg, A., Wichmann, H.-E., Heinrich, J., & German Infant Nutrition Intervention plus Study Group. (2010). Infant-onset eczema in relation to mental health problems at age 10 years: Results from a prospective birth cohort study (German Infant Nutrition Intervention plus). The Journal of Allergy and Clinical Immunology, 125(2), 404–410. https://doi.org/10.1016/j.jaci.2009.10.055
Schmitt, J., Romanos, M., Schmitt, N. M., Meurer, M., & Kirch, W. (2009). Atopic eczema and attention-deficit/hyperactivity disorder in a population-based sample of children and adolescents. JAMA, 301(7), 724–726. https://doi.org/10.1001/jama.2009.136
N. A. Libre. (2021). A Discussion Platform for Enhancing Students Interaction in the Online Education. Journal of Online Engineering Education, 12(2), 07–12. Retrieved from http://onlineengineeringeducation.com/index.php/joee/article/view/49
Sen, S., Duman, R., & Sanacora, G. (2008). Serum brain-derived neurotrophic factor, depression, and antidepressant medications: Meta-analyses and implications. Biological Psychiatry, 64(6), 527–532. https://doi.org/10.1016/j.biopsych.2008.05.005
Palagan Senopati Sewoyo, I Made Kardena. (2022). Canine Transmissible Venereal Tumor: Treatment Review and Updates. Revista Electronica De Veterinaria, 01 - 07. Retrieved from https://www.veterinaria.org/index.php/REDVET/article/view/133
Sharp, S. I., McQuillin, A., & Gurling, H. M. D. (2009). Genetics of attention-deficit hyperactivity disorder (ADHD). Neuropharmacology, 57(7–8), 590–600. https://doi.org/10.1016/j.neuropharm.2009.08.011
Verlaet, A. A. J., Noriega, D. B., Hermans, N., & Savelkoul, H. F. J. (2014). Nutrition, immunological mechanisms and dietary immunomodulation in ADHD. European Child & Adolescent Psychiatry, 23(7), 519–529. https://doi.org/10.1007/s00787-014-0522-2
Wilens, T. E., Biederman, J., Faraone, S. V., Martelon, M., Westerberg, D., & Spencer, T. J. (2009). Presenting ADHD symptoms, subtypes, and comorbid disorders in clinically referred adults with ADHD. The Journal of Clinical Psychiatry, 70(11), 1557–1562. https://doi.org/10.4088/JCP.08m04785pur
Yirmiya, R., & Goshen, I. (2011). Immune modulation of learning, memory, neural plasticity and neurogenesis. Brain, Behavior, and Immunity, 25(2), 181–213. https://doi.org/10.1016/j.bbi.2010.10.015